Citation: I’ons G, “Prefilled Safety Syringe Market Thrives Amid Self-Administration Trend”. ONdrugDelivery Magazine, Issue 105 (Feb 2020), p 86-87.
George I’ons looks at how the growing trend of patient self-administration is driving demand for prefilled safety syringes.
“Needlestick injuries still present a risk to users and their carers in both clinical and non-clinical settings.”
It is well understood that many populations are ageing – for example, by 2030, it is anticipated that there will be more than 21,000 centenarians in the UK, with one in five people aged 65 and over.1 As life expectancy rises, the likelihood of time spent in poor health with multiple chronic health conditions also increases.
At the same time, the gap between the number of clinically trained staff needed and those available is projected to reach almost 250,000 by 2030,2 leaving the existing workforce significantly overstretched. Emerging from the acknowledgement that constraints placed on hospitals by staff shortages, stretched budgets and an ageing population could impact the healthcare system as a whole, the growing trend of home-based treatment as well as patient self-administration is also evidence of a transitioning healthcare landscape.
In the past few years, a wave of biological therapies for patients with chronic conditions has entered the market. These therapies are often the ones to provide the best outcomes for patients suffering from chronic conditions such as neurological, cardiovascular and autoimmune diseases. Their administration, typically via subcutaneous injection, makes them a perfect candidate for self-administration using prefilled syringes.
PATIENT QUALITY OF LIFE
“Medical device manufacturers are key to shaping the future of products for self-administration of injections and should ensure designs have integrated robust needlestick-prevention features.”
Similarly, the frequency of injections required to treat these chronic conditions further increases their suitability for a home environment rather than obliging patients to visit a clinic for every single injection. Home-based treatment can greatly improve patient quality of life and provide support to patients who live far from a hospital or who are less able to travel.3 Providing patients with the tools to self-administer their medication also hands them some power and responsibility to manage their own disease and is effective in helping to reduce the burden on hospitals.
Outsourcing low-risk medical procedures for chronic patients could alleviate some of the pressure on hospitals. However, needlestick injuries still present a risk to users and their carers in both clinical and non-clinical settings. In this sense, the shift of drug delivery towards home environments is a useful reminder that best practices around the safe usage of sharps, including needles, should not only be extended beyond hospital walls but also reinforced in the hospital setting.
Crucially, medical device manufacturers are key to shaping the future of products for self-administration of injections and should ensure designs have integrated robust needlestick-prevention features.The activation and deployment of any needle-shielding feature should factor in the capabilities of all patients and should ideally be an automatic part of the normal use of the device.
HIGH RATES OF INJURY
The implementation of the EU Directive 2010/52/EU more than six years ago for the prevention of sharps injuries has had a positive outcome – yet needlestick injuries continue to occur, including among trained medical staff. A new survey suggests that 94% of practising UK surgeons have experienced a needlestick injury or have witnessed a colleague experience one.4 With such high rates of injury, even within a formal healthcare setting, some of the solution now rests with manufacturers to engineer devices that are not only better suited to self-administering patients but also reduce risks of needlesticks for healthcare practitioners.
Beyond hospital walls, it is estimated that – across all EU economies – the compliance level for safety-engineered injection devices falls from 70% to 60% when moving from clinical to non-traditional settings.5 Needless to say, non-compliance is linked to a higher risk of needlestick injuries occurring and of patients, carers and residential non-users contracting more than 20 possible blood-borne infections. Often unaware of the risks presented by a potentially contaminated device, family lack of awareness makes them highly unlikely to report any exposure or seek treatment or advice – with an estimated 50% of sharps injuries going completely unreported.6
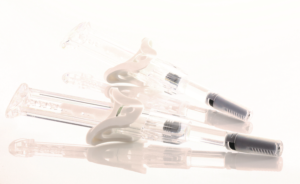
Figure 1: The growing need for prefilled safety syringes is driven by the increasing number of injectable products designed for self-administration.
Unsurprisingly, this backdrop of increasing self-administration has driven a growing need for prefilled safety syringes (Figure 1). Integrating safer features into the design of drug delivery devices may reportedly reduce needlestick injuries and contaminations by up to 80%.7 More concretely, while devices with hollow-bore needles or syringes which retain an exposed needle after use present a heightened risk, retracting and needle-shielding mechanisms are much safer. It therefore comes as no surprise that global spending on safety syringes reached US$772 million (£594 million) in 2018 and is expected to grow by a compound annual growth rate of 8.1%, reaching $1.137 billion by 2023.8
LEVEL OF INDEPENDENCE
More than reducing injuries, prefilled safety syringes must be designed and engineered factoring in the dexterity – or lack thereof – of the patients they may treat. The growing requirement for human factors testing, as well as the need for devices to be intuitive and easy to use, require minimal force to activate and include passive safety mechanisms to reduce additional activation steps, are further influencing the market for prefilled safety syringes.
In conclusion, enabling a wide range of patients to administer their medication safely without professional assistance, safety prefilled syringes are key to unlocking a certain level of independence for patients, whilst also minimising the safety risks typically present during unsupervised administration.
REFERENCES
- Age UK, “Later life in the United Kingdom”. May 2019.
- The Health Foundation, “A critical moment: NHS staffing trends, retention and attrition”. February 2019.
- Bittner B, Richter W, Schmidt J, “Subcutaneous Administration of Biotherapeutics: An overview of Current Challenges and Opportunities”. BioDrugs, October 2018, Vol 32(5), pp 425–440.
- News Medical, “Survey: 94% of UK surgeons have encountered a needlestick injury”. September 2019.
- European Biosafety Network, “Sharps Safety Survey 2016”.
- “Stop Sticks Campaign”. Web Page, US CDC’s National Occupational Health Agenda (NORA). Accessed January 16, 2020.
- World Health Organization, “Needlestick Safety and Prevention”.
- Market Data Forecast, “Safety Syringes Market by Technology.” October 2018.
Previous article
ADDRESSING THE EVOLVING NEEDS OF VARIABLE DRUG DELIVERY REGIMENSNext article
DEVELOPMENT OF A NEW HIGH-PERFORMANCE AUTOINJECTOR
